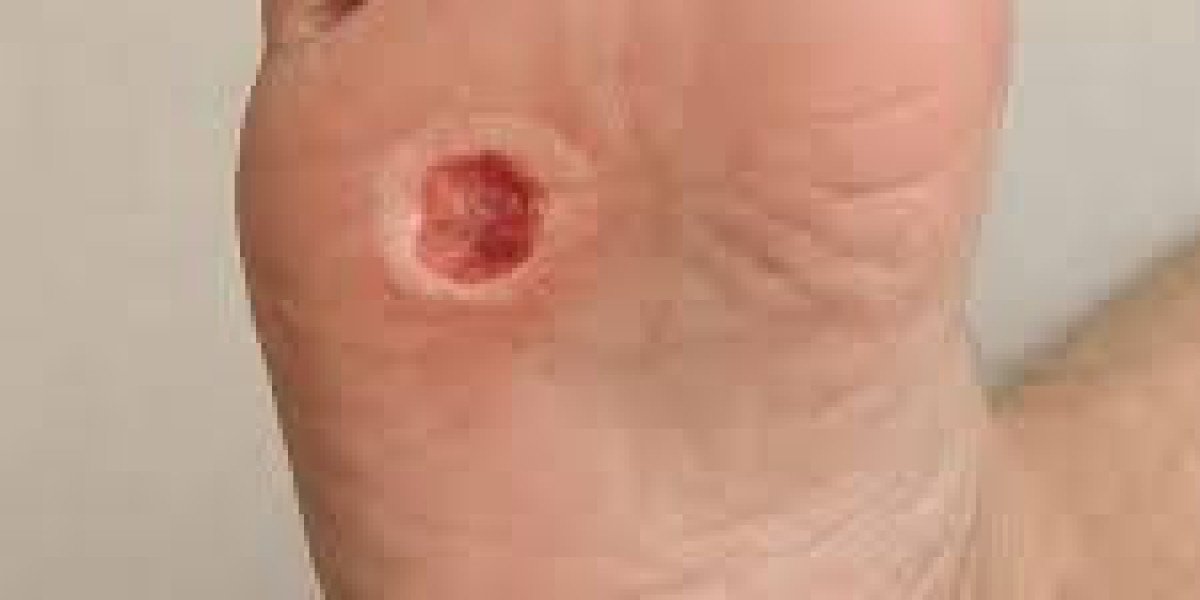
Foot health is often overlooked—until something goes wrong. For people living with diabetes, even a small cut or blister can turn into a serious problem if not treated properly. One of the most dangerous complications is a diabetic foot ulcer, a condition that can escalate quickly without expert care.
Recognizing the warning signs early and seeking help from diabetic foot ulcer specialists can prevent severe infections, long-term damage, and even amputation. In this guide, we’ll walk you through the top signs that indicate it’s time to see a specialist—before it’s too late.
What Is a Diabetic Foot Ulcer?
A diabetic foot ulcer is an open sore or wound that typically develops on the feet due to a combination of poor circulation, nerve damage, and high blood sugar levels.
These ulcers can be difficult to heal and may worsen without proper treatment. That’s why early evaluation by **diabetic foot ulcer specialists ** is critical.
Why Early Intervention Matters
Waiting too long to address foot problems can lead to serious complications. Early care from **diabetic foot ulcer specialists ** helps:
- Prevent infections
- Promote faster healing
- Reduce the risk of amputation
- Improve overall foot health
The sooner you act, the better your chances of recovery.
Top Signs You Need a Diabetic Foot Ulcer Specialist
Ignoring early symptoms can be risky. Here are the key warning signs that should never be overlooked.
1. A Wound That Won’t Heal
One of the most obvious signs is a wound that doesn’t show signs of healing within a few days.
If you notice:
- No improvement in size or depth
- Persistent redness or swelling
It’s time to consult **diabetic foot ulcer specialists ** immediately.
2. Persistent Pain or Discomfort
While some people with diabetes may not feel pain due to nerve damage, others may experience ongoing discomfort.
Pain that doesn’t go away could indicate an underlying issue that requires attention from **diabetic foot ulcer specialists **.
3. Swelling and Redness Around the Area
Inflammation is often a sign of infection or worsening tissue damage.
If swelling or redness spreads, seeking care from **diabetic foot ulcer specialists ** can prevent complications.
4. Drainage, Pus, or Foul Odor
Any discharge from a wound is a serious warning sign.
This may indicate infection, which needs immediate treatment by **diabetic foot ulcer specialists **.
5. Skin Discoloration or Darkening
Changes in skin color, especially black or dark areas, may signal tissue death (gangrene).
This is a medical emergency and requires urgent care from **diabetic foot ulcer specialists **.
6. Numbness or Loss of Sensation
Neuropathy can cause you to lose feeling in your feet, making it harder to notice injuries.
If you experience numbness, regular check-ups with **diabetic foot ulcer specialists ** are essential.
7. Increased Foot Temperature
A sudden increase in warmth around a specific area may indicate infection or inflammation.
Early intervention by **diabetic foot ulcer specialists ** can help prevent further damage.
8. Cracks, Blisters, or Calluses
Small skin issues can quickly turn into ulcers if left untreated.
Even minor problems should be evaluated by **diabetic foot ulcer specialists ** to avoid complications.
9. Difficulty Walking or Standing
Pain or discomfort that affects your ability to walk may indicate a deeper issue.
Seeking help from **diabetic foot ulcer specialists ** can address the root cause.
10. Previous History of Foot Ulcers
If you’ve had ulcers before, you’re at higher risk of developing them again.
Regular monitoring by **diabetic foot ulcer specialists ** is crucial for prevention.
What Happens If You Delay Treatment?
Delaying care can lead to severe complications, including:
- Infections spreading to deeper tissues
- Bone infections
- Gangrene
- Amputation
These risks highlight the importance of timely care from **diabetic foot ulcer specialists **.
What to Expect During Your Visit
Seeing **diabetic foot ulcer specialists ** involves a thorough evaluation and personalized care plan.
Assessment May Include:
- Examination of the wound
- Blood flow testing
- Infection screening
- Review of your medical history
Treatment Options May Include:
- Wound cleaning and debridement
- Advanced dressings
- Antibiotics for infections
- Offloading techniques to reduce pressure
The goal is to promote healing and prevent complications.
How to Prevent Foot Ulcers
Prevention is key to avoiding serious issues.
Daily Foot Care Tips
- Inspect your feet every day
- Wash and dry your feet properly
- Moisturize to prevent cracks
- Trim nails carefully
Choose Proper Footwear
Wear comfortable, well-fitting shoes to avoid pressure and injury.
Manage Blood Sugar Levels
Keeping your glucose levels under control supports healing and prevents complications.
Schedule Regular Check-Ups
Routine visits to **diabetic foot ulcer specialists ** can help detect problems early.
Who Is at Higher Risk?
Some individuals are more likely to develop foot ulcers, including those with:
- Long-term diabetes
- Poor blood circulation
- Nerve damage
- Previous foot injuries
If you fall into these categories, regular visits to **diabetic foot ulcer specialists ** are highly recommended.
The Role of Early Action
Taking action at the first sign of trouble can make a significant difference.
Early care from **diabetic foot ulcer specialists ** can:
- Stop ulcers from forming
- Prevent infections
- Reduce recovery time
Ignoring symptoms, on the other hand, can lead to life-altering consequences.
Final Thoughts
Your feet carry you through life—don’t wait until it’s too late to take care of them. Recognizing the warning signs and seeking help from **diabetic foot ulcer specialists ** at the right time can prevent serious complications and protect your mobility.
If you notice any unusual symptoms, act quickly. Early intervention can save not just your feet—but your quality of life.
FAQs
1. When should I see a diabetic foot ulcer specialist?
You should consult **diabetic foot ulcer specialists ** as soon as you notice any wound, pain, or unusual changes in your feet.
2. Can small foot wounds become serious?
Yes, even minor injuries can worsen quickly, making early care from **diabetic foot ulcer specialists ** essential.
3. Are foot ulcers always painful?
Not always. Due to nerve damage, some people may not feel pain, which is why regular check-ups with **diabetic foot ulcer specialists ** are important.
4. How often should I check my feet?
Daily inspection is recommended, along with regular visits to **diabetic foot ulcer specialists ** for preventive care.
5. Can foot ulcers be prevented completely?
While not always preventable, proper care and guidance from **diabetic foot ulcer specialists ** can significantly reduce the risk.
6. What happens during treatment?
Treatment may include wound care, infection control, and pressure relief, all guided by **diabetic foot ulcer specialists **.