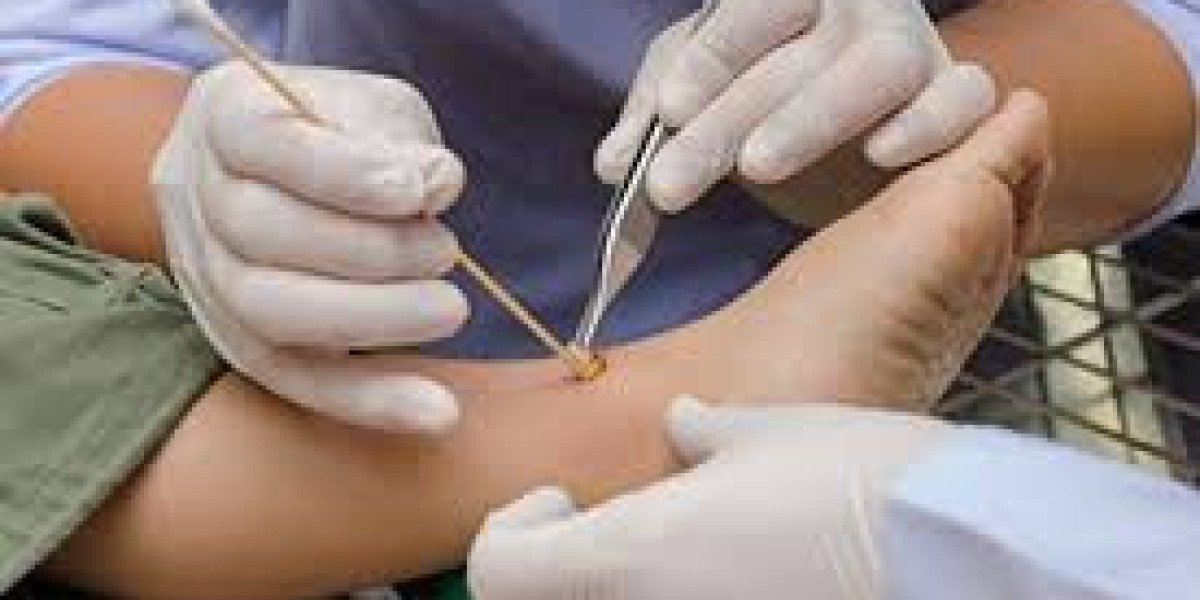
Facing a medical procedure can feel overwhelming, especially when it involves wound treatment. If your healthcare provider has recommended surgical debridement, understanding what the procedure involves can ease anxiety and help you prepare confidently. This comprehensive guide walks you through every stage—from evaluation to recovery—so you know exactly what to expect.
Understanding the Purpose of Surgical Debridement
Before exploring the steps, it’s important to understand why surgical debridement is performed. This procedure removes dead (necrotic), infected, or contaminated tissue from a wound. By clearing away non-viable tissue, the body can focus on healing healthy tissue more effectively.
It is commonly recommended for:
Chronic wounds
Diabetic foot ulcers
Pressure ulcers (bedsores)
Severe burns
Traumatic injuries
Infected surgical wounds
Gangrenous tissue
When wounds fail to heal due to infection or tissue death, surgical debridement often becomes the most efficient solution.
Step 1: Initial Medical Evaluation
The first stage of surgical debridement begins with a thorough wound assessment. During this evaluation, the healthcare provider will:
Measure wound size and depth
Assess tissue color and condition
Check for signs of infection
Evaluate blood circulation
Review your medical history
In some cases, imaging tests such as X-rays or ultrasounds may be ordered to determine whether deeper tissues or bone are involved.
Patients with underlying conditions like diabetes, vascular disease, or immune disorders require additional evaluation to ensure safe treatment planning.
Step 2: Determining the Type of Anesthesia
Comfort is a top priority during surgical debridement. Depending on the wound’s size, location, and severity, anesthesia options may include:
Local anesthesia
Used for smaller wounds. The area around the wound is numbed, and the patient remains awake.
Regional anesthesia
Blocks sensation in a larger part of the body, such as a limb.
General anesthesia
Used for extensive wounds or complex cases. The patient is fully asleep during the procedure.
Your provider will discuss the most appropriate option based on your condition.
Step 3: Preparing the Wound Area
Before beginning surgical debridement, the surgical team ensures a sterile environment to prevent infection. Preparation typically includes:
Cleaning the surrounding skin
Applying antiseptic solution
Draping the area with sterile coverings
Proper preparation minimizes bacterial contamination and improves healing outcomes.
Step 4: Removal of Dead and Infected Tissue
This is the core step of surgical debridement. Using specialized instruments such as scalpels, scissors, curettes, or forceps, the surgeon carefully removes necrotic tissue while preserving as much healthy tissue as possible.
The goal is to:
Eliminate infection sources
Reduce bacterial load
Restore blood flow to viable tissue
Create a healthy wound bed
In some advanced cases, hydrosurgical tools may be used to increase precision and minimize damage to surrounding tissue.
Step 5: Irrigation and Cleaning
After removing dead tissue, the wound is thoroughly irrigated with sterile saline or an antiseptic solution. This step helps flush out:
Debris
Loose tissue fragments
Remaining bacteria
Proper irrigation significantly reduces the risk of post-procedure infection.
Step 6: Hemostasis (Controlling Bleeding)
Minor bleeding is common during surgical debridement, especially when removing necrotic tissue. The surgical team ensures bleeding is controlled using:
Direct pressure
Sutures if necessary
Cauterization in certain cases
Controlling bleeding ensures safe recovery and promotes optimal healing conditions.
Step 7: Dressing the Wound
Once the wound bed is clean and stable, a sterile dressing is applied. The type of dressing depends on:
Wound depth
Moisture levels
Infection status
Amount of drainage
Moist wound healing is often encouraged, as it supports tissue regeneration and prevents scab formation that could delay healing.
Step 8: Post-Procedure Monitoring
After surgical debridement, patients are monitored briefly to ensure:
Stable vital signs
Controlled bleeding
No adverse reaction to anesthesia
For minor procedures under local anesthesia, patients may go home the same day. More complex cases may require short hospital observation.
Pain Management After Surgical Debridement
It’s normal to experience mild to moderate discomfort after surgical debridement, especially once anesthesia wears off. Pain management strategies include:
Prescribed pain medication
Over-the-counter pain relievers
Elevating the affected area
Avoiding pressure on the wound
Most patients report manageable pain that improves within a few days.
Recovery Timeline
Healing time varies depending on wound size and patient health.
First Few Days
Mild swelling
Slight tenderness
Drainage that gradually decreases
First Few Weeks
Formation of healthy granulation tissue
Reduced redness
Gradual wound contraction
Complete Healing
Small wounds may heal within weeks, while larger wounds may require months of ongoing care.
Patients with chronic conditions may require repeated sessions of surgical debridement if new necrotic tissue forms.
Benefits of Surgical Debridement
The structured, precise approach of surgical debridement provides several advantages:
Immediate removal of necrotic tissue
Faster healing compared to conservative methods
Reduced infection risk
Improved antibiotic effectiveness
Preparation for skin grafting if necessary
This proactive approach can significantly reduce long-term complications.
Risks and Possible Complications
Although generally safe, surgical debridement carries some risks, including:
Temporary bleeding
Post-procedure infection
Pain or swelling
Rare damage to healthy tissue
Careful surgical technique and proper wound care minimize these risks.
How to Prepare Before the Procedure
To ensure a smooth experience with surgical debridement, patients should:
Inform providers about medications
Discuss allergies
Follow fasting instructions if general anesthesia is used
Arrange transportation if sedation is administered
Being well-prepared reduces stress and improves outcomes.
Home Care Instructions
After surgical debridement, proper wound care is essential. Patients are typically advised to:
Change dressings as instructed
Keep the wound clean and dry
Avoid strenuous activity
Monitor for signs of infection
Attend follow-up appointments
Nutrition plays a key role in healing. Adequate protein, vitamin C, zinc, and hydration support tissue repair.
When to Contact a Healthcare Provider
Seek medical attention if you experience:
Fever
Increasing redness or swelling
Excessive bleeding
Persistent foul odor
Severe pain
Prompt evaluation ensures early management of complications.
Psychological Reassurance for Patients
It’s common to feel anxious before undergoing surgical debridement. However, understanding that the procedure is designed to remove harmful tissue and promote healing can provide reassurance.
Many patients report significant improvement in wound appearance and comfort shortly after treatment.
Long-Term Outlook
The long-term success of surgical debridement depends on:
Consistent wound care
Managing underlying conditions
Proper nutrition
Regular follow-up visits
With appropriate care, most wounds show substantial improvement after the procedure.
Conclusion
The step-by-step process of surgical debridement is carefully designed to remove dead tissue, reduce infection risk, and restore the body’s natural healing ability. From initial assessment to recovery, each stage plays a critical role in achieving optimal outcomes.
Understanding what to expect can help patients feel confident and prepared. If recommended by a healthcare provider, timely surgical debridement may be the key to preventing serious complications and promoting faster recovery.
FAQs
How long does surgical debridement take?
The procedure can take 30 minutes to a few hours depending on wound size and severity.Will I need stitches after surgical debridement?
Most wounds are left open to heal naturally, but some cases may require sutures.Is hospital stay required?
Minor procedures are often outpatient, while complex cases may need short hospitalization.Can I walk after surgical debridement?
It depends on the wound location. Your provider will give activity guidelines.How many sessions might be needed?
Some wounds require multiple sessions if new necrotic tissue develops.Is the procedure safe for diabetic patients?
Yes, but blood sugar control is crucial for proper healing.